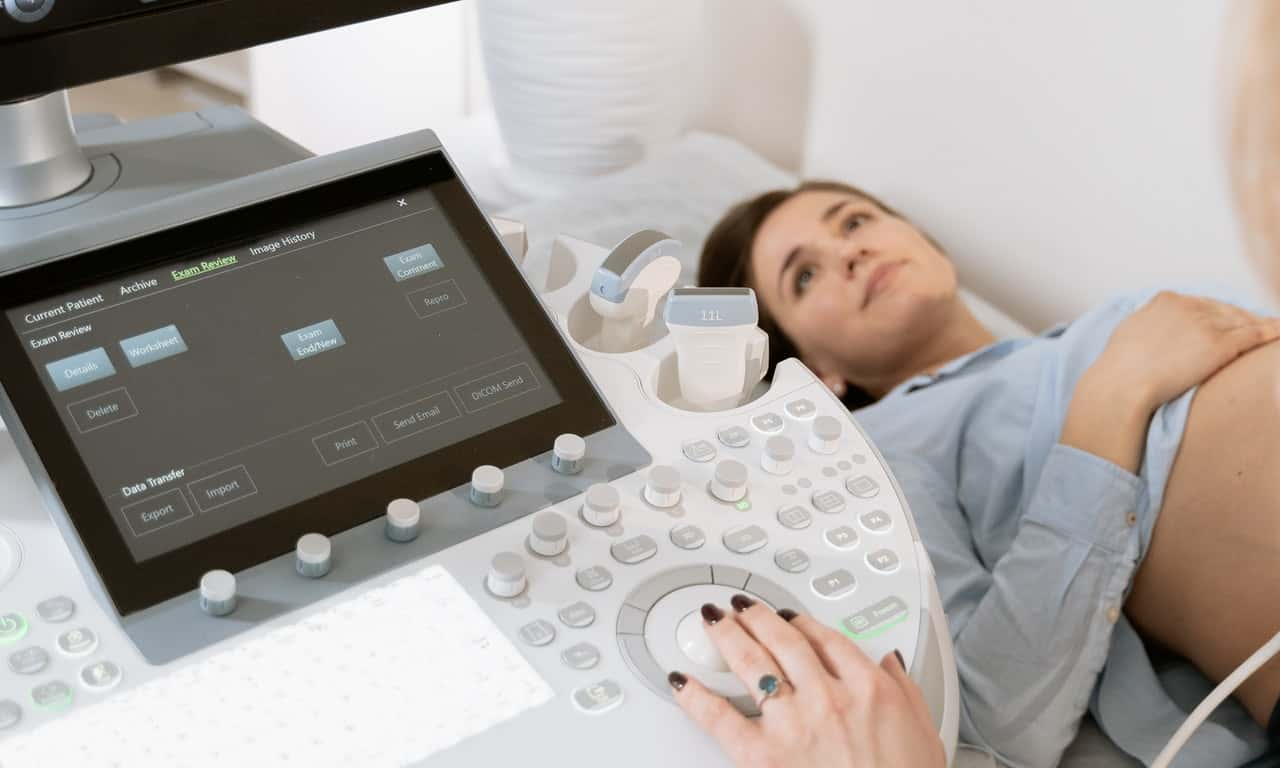
From horrifying medical mistakes to shocking survival stories, these medical "OMG" moments are sure to send a chill down your spine.
1. A Leg Down
My grandfather’s friend needed to have his leg amputated. Somewhere between him leaving the hospital bed to go into surgery and coming back out, a horrible mix-up happened. Someone had mislabelled the leg and they amputated the wrong leg.
He went back into surgery three days later—he’s very old and they were worried about him going under once let alone twice—and they removed the other (correct) leg. This is one of those stories that I couldn’t believe until I actually met the guy and realized he really does have both legs amputated, for no good reason other than negligence.
2. More Than A Stain
I’m an eye doctor, and many people don’t realize that diabetics need to have their eyes checked regularly. After all, a diabetic complication can result in blindness. I had a patient 15 years ago that was experiencing severe diabetic vascular changes against the retina and required laser intervention. On the day of her surgery, she chooses to go to work instead. It was the worst mistake she could possibly make.
She worked in the cleaning industry, and on that day she inhaled some of her cleaner fumes. They caused her to sneeze, which spiked her blood pressure, and she blew the fragile blood vessels in both of her eyes wide open. Immediately, she’s blinded in both eyes in a matter of seconds.
3. A Quirky Defect
When I was a medical student, a patient and his brother came in together. The patient was just there for a post-op visit after a hernia repair. Turns out, after inspection, he actually had another baseball-sized hernia. Somehow, that’s not the craziest part. His brother, on the other hand, LITERALLY had a football-sized hernia visibly coming out of the left leg of his shorts.
It looked like an inguinal hernia, and he was able to use it as an armrest. I asked him if that bothered him at all, and he just straight up said: "My brother's hernias were painful but this isn't, so I thought it was just a quirky defect". I hope he was lying to save face, but we recommended he get it taken care of.
 Shutterstock
Shutterstock
4. Glitches In Time
I was rushed to the ER after frequent blackouts and sudden-onset fatigue. I worked a physical labor job and attended college after my shift, so I didn't think anything about the fatigue and the blackouts. I thought it was just my brain giving me a fast forward through mind-numbing tasks.
Typically, I would have blackouts while driving because my commute to work was about 45 minutes and my school was about an hour away from my work. I can’t believe how dangerous it was. I would get on the highway, blink, and the next thing I knew, I was in the parking lot with 45 minutes having passed in an instant.
I told my girlfriend about this and she told me something was wrong; but being a dumb 19-year-old, I ignored it. It wasn't until I was at work stacking chairs that it really started to sink in—I had an empty cart, put a chair on it, turned around to pick up another chair, then turned back to a chilling sight.
The cart was full—but I didn’t remember filling it. When I saw the full cart, it was like someone hit me in the back of the head and I instantly felt like I hadn't slept in days. I ended up sitting down and one of my co-workers noticed I was white as a ghost. The guy in charge forced me to go to the hospital even though I insisted I was fine.
Once I got to the hospital and got brain scans done, it turned out I was having mild seizures caused by a lack of sleep. When I told the doctor about my commuting blackouts, he looked like he just saw a ghost. He told me he had no idea how I didn't crash. He basically told me to find a new job and get more sleep.
5. No Laughing Matter
One night I had a young guy; a walk-in who thought it was hilarious he had a stab wound. He arrived at 3:00 am and had been waiting hours before deciding to get help. He also brought in his family and friends who also didn’t think it was a serious injury. During his evaluation, it registered as a level one and his blood pressure was low.
His heart rate was soaring as his body tried to compensate for the loss of blood. As soon as we brought him into a room, he coded and never woke up. We tried to revive him with a manual cardiac massage, which meant cracking his chest and manually pumping the heart. The blade had nicked his abdominal aorta, which ruptured. But that wasn't the most chilling part.
When we went back to the waiting room, his friends and family were having a pizza party, not recognizing the fatal status of their loved one.
6. Spick And Span
I’m a surgical tech, and we were doing a skin graft on a burn patient. In those types of surgeries, you have two different operative sites if you're taking the skin graft from the patient and not using cadaver skin. This means I have two different surgical teams going and only one me bouncing back and forth and assisting both teams.
This was also at a university hospital, meaning I have attending surgeons, residents, and medical students all working alongside me. If you work in surgery, you know that unless you're the tech, YOU DO NOT TOUCH THEIR TABLE OR ANYTHING ON IT.
As we're doing the skin harvest, you have to keep the skin moist until it's ready to be transplanted on the site. I wrap mine in damp sponges and keep it on my table. I bet you can see where this is going. I turn back to my table and the sponge WITH THE SKIN IN IT is gone.
I look everywhere and finally stop everyone from working to ask who has the damp sponge that was on my table. A resident told me my table was "too cluttered" and he threw the sponge in the trash. I saw red. I've never had to scold a doctor so badly in my life.
Not only did he touch my table, he threw away an item that needs to be accounted for after surgery, and it had a specimen in it. Since the skin was no longer sterile, we had to use cadaver skin, and you know who pays for that? The PATIENT. So, a note to all the baby docs, please don't touch your scrub's table unless we okay it.
7. A Little Too Late
I’m a nurse with twenty years of experience and a master's degree. This lady had a non-healing, large wound on her left chest area for six months and painful axillary nodules that she had for six years prior to the wound. Any non-healing wound is immediately assumed as cancer until proven otherwise. Well, this lady had stage four, untreatable cancer—all for a heartbreaking reason.
She just wasn’t taught that cancer was treatable. The patient told us, “I wish they could do something for breast cancer, and cancer in general". Clearly, she was not informed about how most women with painful nodules should come in ASAP as the cancer is most treatable when detected early. She passed on three weeks after her diagnosis.
She was sedated for about two weeks and five days after diagnosis because that’s how she wanted to go. At least she wasn't in pain, and was pretty much asleep for all of it.
8. I'm Not Crying Wolf
One night, when I was 16, I had a very sharp pain in my right side. I tossed and turned for a couple of hours before getting up and knocking on my mom’s bedroom door; a forbidden action. My mother swung the door open and snapped at me. Then, when I explained my pain, she told me it was just heartburn.
She ordered me to drink some milk and go back to bed. I drank the milk, tossed around my bed for a few more hours, and finally passed out from exhaustion. The next day and a few weeks after that, I felt fine. But then, a couple of months later, the pain was back and I woke my mother in the middle of the night again.
She gave me the same response as the first time, and I once again just passed out from exhaustion. Because it was starting to become a pattern, the next time I felt the pain, I didn’t bother going to my mother and just rode it out. This continued until I was 18. Little did I know, it was about to turn into my worst nightmare.
My parents were out of town one weekend and the pain came back worse than ever before, waking me from a deep sleep. After hours and hours of utter agony, hurting to move, hurting to lay still, I broke down and called my mother. On the voicemail I left her, I told her that I thought I was dying.
I finally passed out as the sun began to rise. I was woken up by my uncle banging on the front door and he took me to the doctor, who then referred me to an ultrasound and a surgeon. I was able to get the ultrasound done on the same day but the surgeon didn’t have availability until the end of the week.
I didn’t think anything of it as, once again, the pain had disappeared by then. My mom begrudgingly took me to the appointment with the surgeon, but I’m pretty sure she thought I was faking it since I’d been completely fine all week. I remember sitting in the office with the surgeon, just chatting while we waited for the nurse to bring him my ultrasound file. I’ll never forget when she handed it to him.
He opened the folder and the smile immediately fell from his face. Surgeon: Did they give you any pain meds when you went to the doctor? Me: No, just some antibiotics. Why? Surgeon: Nancy, call my 2 pm and tell them we have to reschedule as I’ll be doing emergency surgery. You should have been sent to me last week. I’ll meet you in the ER.
So yeah, my gallbladder had apparently been filled with stones since I was 16 and it kept making more for the next two years. The surgeon said he’d never seen anything like it. All of this could have been avoided if my mother had just listened to me when I first complained to her.
9. Measure Twice, Cut Once
I work in the pathology lab where the hospital sends all the specimens. One day, a surgeon did a double mastectomy based on a different hospital’s pathology report. The report said the woman had the kind of cancer where both breasts need to be removed. But when we examined her specimens, we made an utterly disturbing discovery.
We found zero cancer in either mammary. Obviously, the surgeon was beside himself and made us look through both mammaries IN THEIR ENTIRETY...It’s unheard of to submit all the tissue like this, but he needed to find cancer. I’ve never seen a surgeon stand there and watch the pathologist like this guy did. We all felt so bad for him and of course the patient.
He was so upset, cussing up a storm the whole time and screaming about “This is why I never take outside pathology reports!” Turns out, the other lab had mislabeled her tissue, so some other lady got the all clear who had cancer, while she lost both her breasts when she didn’t need to.
All around a horrible situation, and the surgeon was sick over it all.
10. Dignity Discourse
A young woman in her 20s comes in with an infected heart. Her infection and heart failure are pretty much past the point of recovery. Her only option was IV antibiotics, hope they work, and plan for hospice care. Her IV lowered the infection but the heart and valve damage were extensive. It was so extreme that the heart was producing micro-clots.
After the micro-clots, her fingertips went purple and clots migrated to her lungs. When she arrived in my ICU ward she was struggling to breathe. At this point, she decides to fill out a DNR or Do Not Resuscitate and move into hospice care. Unfortunately, our state has a loophole where if the patient becomes unresponsive their proxy can change the DNR. Sadly, the worst happened.
Her mom went to court and was granted healthcare proxy rights. This meant once the daughter was disoriented, her medical decisions belonged to her mother. The first thing her mom did was cancel the DNR, and our team was forced to put her on life support. The consequences were horrifying.
She as on life support for months and her arms and legs became purple, black, green, then necrotic. Her organs were failing and the clots had traveled to her brain. She was unresponsive and we knew it shouldn’t be prolonged.
We took the case to risk management, we held ethics meetings, and we went to court against the mother to revoke her healthcare proxy to fight for the patient's right to die with dignity. The court refused and the mother stayed in control.
11. The Root Of The Problem
My husband and I were messing around and he chased me through the kitchen. When I took a hard left turn, he lost his footing and fell on his side. He’s a big dude, so falling is a bit more dramatic for him. He couldn’t put pressure on his leg and he knew immediately he was hurt pretty bad.
He was able to crawl to the couch, and once he settled in, he said he wasn’t in too much pain. He decided to sleep on the couch that night so he wouldn’t have to go upstairs. We made an appointment in the morning for the ER so we wouldn’t have to sit there all day, but they didn’t have an opening until 2 pm, so we just hung out at the house.
He was in a decent amount of ambient pain, but it didn’t seem too urgent. Once we got to the hospital, however, we found out the shocking truth. He had broken his hip, breaking off his entire ball joint from the top of his femur. The nurses said they couldn’t believe that he was able to sit up and sleep on it, which implied that we should have come the night before—and probably by ambulance.
It required surgery with some hefty bolts to put it back into place. But the crazy part is that, apparently, a healthy 30-year-old man breaking his femur from standing is highly unusual. That’s when we found out that there was an even more terrifying cause behind it.
After several tests and an MRI, it turned out he was in the early stages of osteoporosis. Even craziest? It was due to a pituitary tumor in his brain. So we discovered a benign brain tumor all because the dude was wearing slippery socks.
 Shutterstock
Shutterstock
12. Don’t Skip The Important Stuff
When I was an anesthesia resident, a pregnant woman came into our medium-sized community hospital in the night with some abdominal pain and nausea. Her doctor determined she was not in labor so we just treated her with medication and kept her overnight. In the morning, a new obstetrician started daily rounds. When he saw her, he immediately raised the alarm.
The new obstetrician noted that the patient's blood pressure had dropped. They felt the patient's uterus and it was exquisitely tender. At this point, our patient is feeling very faint. Now the diagnosis is likely a uterine rupture, which is when a small hole has burst in the womb. In these cases, the solution is an emergency C-section, and my team was called in to perform this delivery.
A uterine rupture is bad enough, but when we removed the tiny preterm baby, we discovered a horrific truth. It wasn't a rupture but a placenta percreta. That's when the placenta grows through the wall of the uterus and into the surrounding organs, in our patient’s case her bladder. The surgery became more complicated and we had to call for help.
In the OR we now had a urologist, and two other anesthesiologists and started a blood transfusion as she had lost a lot of blood. This condition is usually detected on a prenatal ultrasound, but the patient had skipped hers. If she hadn’t missed it, this surgery would have been performed in a big city due to its risky and delicate nature. Thankfully, mom and baby were OK.
13. Up In Smoke
My patient was a teenage girl who was taking a nap at home. As she slept, a reckless driver crashed into her house, causing an electrical fire, igniting a ruptured gas line, and setting the entire house ablaze. Originally she got out with her sister, but went back in to try and rescue her dad and dogs. When firefighters pulled her out, her body was 95% burned.
When she arrived in ICU we registered smoke inhalation, lung damage, carbon monoxide, and cyanide poisoning plus toxic inhalation. She survives the initial presentation to the trauma unit and now she’s in our burn unit, and it’s only going to get worse before it gets better. The only intact skin on her body was a small area around her inner thigh.
Her hair, face, eyelids, and lips are gone. We do what we can with moist sterile dressings and debridement plus broad-spectrum antibiotics. At the end of the day, she looked like a mummy fully wrapped by the end. There is no chance of her having a normal life ever again. The chances of her surviving are in the single digits. After a few days, the infection begins to set in.
All that damaged tissue was a breeding ground and the first thing we noticed was the smell. The only thing you can really do to encourage healing at that point is IV/Topical antibiotics and debridement. Basically, large wounds heal better when they are scraped or shaved to expose the wound bed. This removes dead cells which hamper growth and encourages new skin formation.
It takes weeks of treatments, and we had to do this all over her body. This was scheduled multiple times per week. One day, I said out loud in the OR, “This is the worst thing I’ve ever seen in my life". Several years in medicine later that statement remains true. She survived the next few days, and we started with the skin grafts. Trying to rebuild her face, and cover her body.
Her average surgery time was about 10 hours per procedure. We have to keep the room at 98 degrees because burn patients go hypothermic quickly. This meant 10 hours in full scrub gear at nearly 100-degree heat.
14. Puff-Puff-Pass-Out
I once had a middle-aged female patient, with no prior medical history, who was flown in from another state for escalation of care. She was transferred for intracranial hemorrhage. But one thing made her case stand out. According to her family, it had happened after she tried the green stuff for the first time.
She had taken a big, long toke and she coughed so hard that it ruptured a vessel in her brain. She survived her surgery, but during her post-op recovery her heart stopped and she went into cardiac arrest. I attended the code blue with the team, and with rapid sequence intubation and CPR, we were able to bring her back. But that wasn't the end of it.
After she was stable I was outside the room reviewing my patient list when she went into cardiac arrest a second time! The same team had to sprint across the hospital again to handle it. I've never seen the code blue team so out of breath. In one night she was flown in, had a ruptured aneurysm, a hemorrhagic stroke, and two cardiac arrests back to back and lived.
She was a fighter but I hope her family understands no means no next time!
15. In The Blink Of An Eye
This patient had a history of kidney cancer but was in remission. On his latest scan, there was surprising news. There's a focal mass on one kidney. Still, if it’s actually just a focal lesion we can chop off the tip of his kidney and cure him while retaining most of his kidney function. The lead surgeon requests better imaging, so we send him to radiology.
When radiology calls us back with the results and it was the worst possible outcome. The cancer is back and has spread into the renal veins. This takes our patient out of remission and into stage three. The radiologist also mentions he sees shadows in the liver and brain. After the dust settles, everyone agrees that this patient is more advanced and surgery is no longer an option.
The worst part was telling him. Remember, this patient came in thinking he was having a short surgery and leaving completely cured. Instead, the surgeon walks in and says, “I’m sorry, but your cancer has spread and you most likely have about six months to live". His son was five years younger than me and standing next to his dad at the time.
16. Evil From Within
One time, we had a woman come in through the ER with excessive bleeding three weeks after childbirth. That's fairly unusual timing and I took her to surgery for a dilation and curettage, or D&C. I expected to find a little retained placenta and that the bleeding would improve as soon as I got it out. This couldn’t be further from the truth.
As soon as she was on the table, it only got worse. We eventually performed a uterine tamponade balloon. This is a big balloon you fill with saline inside the uterus to apply constant pressure. With medication, we finally got the bleeding stopped and she did ok after a blood transfusion. In total, she lost 1,000cc in the ER plus another 2,000cc in surgery.
Her lab results never showed any retained placenta, meaning her uterus just tried to murder her that night. It’s incredibly rare and I’ve never seen this since. She took the time to send me a thank you card a few weeks later with a handwritten note in it: "Thanks for saving my life, I guess". I kept it in my locker for a while and wish her a happy uterus future!
17. A Heavy Burden
I went to the doctor to get a note for a day off work because I didn't feel so great. The doctor poked me in the stomach and said, "That's not normal," then sent me off to have a scan…which took me two months to get around to. Two weeks later, I got a letter from the doctor asking me to come in. When I got there, the doctor went off at me for not coming in sooner...
He told me to go home, pack a bag, and make my way to the Royal Brisbane immediately as it might be cancer. Some more scans later and it was determined not to be cancer, but a four-kilogram cyst. My only symptom was an enlarged stomach and the "You're getting fat" comments from my mother.
18. Ignoring The Pain
There are so many, but perhaps one of the most stunning cases was the man who thought searing pain while urinating every once in a while was normal. He would have tremendous back pain for a day or so, which he thought was due to advancing age and the highly physical nature of his job. Not incredibly unreasonable, but something he should have still checked out.
Usually, a few days later, he would have searing pain while urinating, then be fine again. Of course, it turned out to be chronic kidney stone formation. He said he never noticed the stones coming out because he never looked down while urinating. Honestly, I still don't understand.
I have had kidney stones myself and it definitely feels like something solid is coming out. Baffling.
19. Without A Leg To Stand On
I was a resident in the ICU and we had a patient recovering from Steven-Johnson Syndrome, which is a rare drug reaction where skin blisters uncontrollably. At the same time, he had a clotted femoral pseudo-aneurysm that was at risk of bursting and bleeding. Between the afternoon and evening rounds, this patient’s nurse asked me to assess his leg swelling.
His whole body was swollen because of all the blisters and he had fluids he'd been getting for his blood pressure. When I checked his right leg, it did look more swollen than a few hours ago and the skin was worse. However, the aneurysm was stable on the ultrasound earlier in the day so it didn't seem like there was much to do other than keep it well dressed and monitored.
A couple of hours later, my co-resident and I are doing our evening rounds as the general surgery team is assessing a few doors down. The leg looks even worse than earlier and is another few centimeters swollen. Even with the swelling, his vitals are stable and he’s receiving the right treatment. We were scratching our heads when the unthinkable happened.
His leg burst. Where the swelling had occurred has now split open and is gushing. The nurse and my co-resident throw on gloves and apply pressure while I grab a surgical kit and try to find the source. Our team is running down the hall to grab the surgeons who are still evaluating patients.
Within two minutes, there's a small team searching through this man’s leg, looking for the cause. Another minute or two later and they've found they found the ruptured vein. They stopped the bleeding as best they can. I think on the repeat blood work that evening he'd lost maybe 10-20% of his blood in five minutes. Now we had to treat the infection.
This patient was pretty frail and had already had a near-fatal reaction to one class of antibiotics. I wish I could say it was a happy ending, but his wound became purulent and he developed bacteria in his blood. It was a bad day that got worse with all the other medical problems he was having. It was just too much and we transferred to palliative.
I’ll never forget the experience and know my team kept him as comfortable as possible.
20. Just Bumming Around
Our patient had a pilonidal cyst that bothered them for years. This is the type of cyst that can be very large at the cleft of your backside, and is caused by hairs that burrow deep under the skin. It flared up while the patient was sitting for long periods, and became inflamed and infected. Normally we would recommend a surgeon for this procedure.
When we examined the cyst, we could see it had opened on its own and was beginning to drain. When I took a closer look, I could see the nest of hair in this opening and my curiosity and an absolute need to remove it took hold. But I had made a fatal error. I didn’t predict the nest acting like a plug, and the removal released the most foul-smelling pus.
Thankfully due to protocol, I was wearing a face shield but it did land on the bridge of my nose and eyebrow. I will never forget the sheer force, trajectory, or smell, but would do it all again if I had the chance. Chalk up my fascination to too many episodes of Dr Pimple Popper. Even so, I still wasn’t prepared for the results.
21. Not One, But Two
My oldest son was 11 years old and he needed a physical for youth tackle football. He had complained that his ankle hurt during the middle of baseball season so she asked if he could take off his shoe. When he did, she immediately pointed to the side of his foot where there was a strange bump, and informed us he had a broken foot.
I didn't believe her because he had the same thing on his other foot as well. So she took a look at the other foot and said, "Oh...he has TWO broken feet". She then sent us over to get X-rays from the hospital. I was laughing in my head, thinking it was so crazy that my son, who not only finished playing in a baseball tournament but had also been running and jumping at the swimming pool literally an hour before, had two broken feet.
After the X-rays were completed, my smile quickly faded as the doctor was right. That's when we learned about how completely flat feet can be damaged with stress fractures that go undetected. He was put into a cast for eight weeks and was made to wear special shoes and insoles for the rest of his life. His feet are still deformed, but it has never slowed him down.
22. A Hairy Situation
This one was actually from back when I was a medical student, but it’s still the weirdest thing I’ve seen. It was my last rotation in medical school before graduating and starting residency. I had completed all my requirements and just wanted to take a few interesting electives of things I hadn’t seen yet. This was a dermatology rotation at the VA.
The rotation had been interesting and chill, and I was seeing my third-to-last patient as a medical student. The guy came in and the resident asked him why he was there. He said, “I have hair coming out of my hand". I figured he meant a weird mole with some hair coming out, but this guy (who was probably in his late thirties or early forties) said, “No, the hair is coming out from under the skin".
The resident asked him what he did for a living and he said he was a barber. Apparently, it’s not too uncommon for hair to poke through the skin, especially for barbers who cut men’s hair. It’s short, thin, and can be kinda pokey after all. It was sort of like getting a sliver, but with hair. But the guy said, “No, it’s a lot of hair, look!”
He held up his hand, making a fist, and there were several hairs poking out from between the knuckles of his pointer and middle finger. I stared in confusion, and the resident grabbed some tweezers to pull out maybe a half dozen short black hairs. The guy said, “Yeah, I already pulled out like 50". That's when the resident's face dropped.
We numbed up the backside of his hand between the first and second knuckle and made a little incision. We were shocked at the mass of hair that we uncovered. We started pulling out GOBS of short black hair. A chunk of 20, a chunk of 30, etc. At some point, she got the magnifying glasses out with an attached light and said, “Oh my gosh, there are still more in there! Sir, do you know how all this hair got into your hand?” His answer was so disturbing, it’s unforgettable.
The guy said, “Oh it probably came in through there!” He flipped his hand over to reveal a HOLE in the palmar aspect of his hand’s skin. It turns out, the dude had cut himself like TWO YEARS before this, and it had never healed properly (he was diabetic), so he just kept cutting hair with this open wound on his hand. Probably every day, a few hairs got stuck in his hand. For two years.
Now those hairs had tunneled through the webbing between his first and second fingers from the front of his hand and out the backside. We spent like 30 minutes MILKING his hand and fingers while more and more hair came out. She said, “There’s no way I got it all out, so you have to come back every two weeks for a few months for us to keep removing more hair from your hand".
23. Unorthodox Wincing
I got a new OB-GYN and went for a check-up. I braced myself for the horrible pain, and she immediately stopped. As it turns out, extreme pain down there ISN'T normal, but I'd just had three other OB-GYNs who apparently didn't care that I cried in pain every time I was checked.
She called it vulvar vestibulitis, but the most commonly used term now is vulvodynia. Apparently, there's no known cause, but some doctors think it may be due to having too many nerve endings in the area. I am doing somewhat better now thanks to some physical therapies and a lidocaine ointment that I can apply beforehand.
24. Tainted Smile
I work at a dentist’s office. A patient came in for an exam, concerned that a part of her tooth was chipped off. On examination, it was not a chip, but rather a piece of calculus, which is the build-up of hard tartar that covers your teeth over time when you don’t brush them. It can be small deposits, or in this case, an entire “bridge” covering her actual teeth.
She thought the calculus was tooth material and was quite shocked to learn we were actually unable to see her real teeth. We gave her an extensive cleaning to remove it all.
25. I Hope This Isn’t Personal
I have Crohn's disease and spent the majority of 2012-2015 going in and out of hospitals due to malnutrition, anemia due to blood loss, an inflamed colon, infections, etc. No medications helped calm my disease down. As a bonus, I got something called Pyoderma Gangrenosum two months after I was diagnosed with Crohn's.
Pyoderma Gangrenosum gave me several open wounds on my legs that were painful and required wound cleaning twice a week with high doses of pain medication. Due to building a resistance, I went from 5mg to 20mg over the course of a year and a half. My daily prescription was valium 5mg and morphine 10mg five times daily to manage the pain.
Under one of my many hospitalizations, I was sent to a bigger hospital than my local one, since they had better resources, equipment, and a special ward for people with gestational issues like mine. A couple of weeks into my stay, I got into big trouble. My stomach was hurting a lot more than usual. I also stopped making bowel movements, which was a big red flag.
I was still going to the bathroom like 50 times a day to pass blood and minuscule amounts of waste, but then stopped overnight. I informed the nurses and spoke to the doctors when they had visitation, but I was getting brushed off by everyone. I asked to be checked out, showing my stomach, which by now looked like a six-month pregnancy.
Regardless, doctors did nothing more than feel my tender stomach daily. I started crying a lot, could hardly sleep, and stopped eating the first or second day because of the pain. Eventually, I was vomiting and overall deteriorating. After six days, I had enough, and finally, someone wheeled in an ultrasound machine to my room.
After a quick look in my stomach, I got a meek, "Oh, your intestines are twisted around on themselves, you need surgery". The next morning I was on the operating table and ended up having my whole large intestine removed because of the extent of damage from the twisting and inflammation. I now have a permanent stoma to function.
The reason they did nothing for a week despite my daily complaints was the doctors thought I was addicted to my pain relief medications. They thought I was complaining for more medication...even though I never asked. The doctor responsible had never interacted with me face-to-face and made the decision based on my medical history alone.
26. The Denial Is Strong
As a teenager, I was listening to my best friend complain about her bad periods. She snapped at me and asked why I didn't care that she was in so much pain. I basically told her that we all go through it every month: "Everyone bleeds through tampons every hour or so. Everyone hurts all the time. Everyone gets the few moments where it's so painful you can barely stand. Everyone does this for eight days".
She looked at me like I was crazy and said no, that's not normal. I argued and said it's exactly how it is for me...it sucks but what can we do? She gently assured me that what I had just told her was not normal and that I should probably see a doctor.
27. Wrong Self-Diagnosis
We learned of a medical case involving a man who had a rash on his foot. He googled it and decided it was eczema or some similar inflammatory disease, so ordered and applied a steroid cream. For those who don't know, those kinds of steroids act by dampening the immune system—the overactivity of which is the cause of diseases like eczema and psoriasis.
However, he, in fact, had a fungal infection and was just reducing his body's ability to fight it off. If I remember correctly, by the time he got to the doctor's, he needed it amputated.
 Unsplash
Unsplash
28. The Family Jewels
My 13-year-old son complained to me that he was unbearably itchy down there. I figured probably sweat, so I told him to wash the area thoroughly and make sure to dry well. A couple of days later, he said it was still itchy and getting bigger. Bigger? He said there was no pain or anything, but it was still itchy and swollen. I still didn't think it was anything more than a sweat rash that maybe needed some ointment.
But when we went to the doctor, we were sent off for an ultrasound. The scan showed zero blood flow to the area, so he was immediately transferred to the emergency room. He went in for emergency surgery where the urologist removes one necrotic mass. It had become randomly twisted and passed at least a week prior. The swelling was a major infection setting in, which also caused the itchiness and swelling.
He had no pain whatsoever and the doctor said that was amazing. For most boys, torsion feels like being kicked in the nuts continuously, and by the infected stage he was in, he should have been screaming and crying from the pain. If we had waited any longer, he could have developed sepsis. He had a follow-up surgery a month later to insert a replacement part and to stitch his remaining one in place so it doesn't happen again.
29. The Circle Of Life
My brother is a paramedic, and he said every time, practically without fail, dispatch would downplay the calls. So one call he had was for a girl "with minor bleeding". He arrived and found her 14-year-old brother frantic. His 12-year-old sister was bleeding everywhere and wouldn't stop. My brother braced for a major cut and expected a blood bath.
Instead, the girl was terrified she was a goner....because of all this blood coming from between her legs. So yeah, that became quite clear quite quickly. She was in the bathtub and he calmed her down and asked them both where their mother was. They called the mom at work and she got on the phone to explain to her daughter what was happening.
When she was passed back to my brother, she asked if ambulances had sanitary pads, but they don’t carry them. He did however use gauze to make a temporary pad and explained to the girl what to do. The mom ran into the house 20 minutes later, thanked my brother profusely, and hugged her daughter for a long time. He never expected to teach someone about the menstrual cycle.
30. The Digit Details
We had a patient call our clinic and say they cut their hand. They wanted to know if we were busy or had time for a couple of stitches. They failed to mention that they were working with a table saw, and had nearly cut off three fingers. Their tendons were exposed and severed, and I sent him immediately to the hospital. He received a hand specialist and kept his digits.
31. Ride-Along-Astray
As an EMT trainee, in my first ride-along we responded to a call where a guy fell at a skate park. When we got there he was conscious, walking, and talking coherently. He hadn’t been wearing a helmet when he fell and a bruise was forming above his eye. With no scrapes and his pupils dilating, we assumed it was a concussion and black eye.
We talked him into coming with us to the ER just to double-check. We get him in the ambulance, lay him down, and his blood pressure had gone down significantly since our first check. Then it took a very dark turn. It escalated quickly to him getting drowsy and throwing up blood. We turned on the sirens and started fluids, but his blood pressure kept dropping.
He was unconscious by the time we got to the ER. Skipping the bruise meant we hadn’t felt the soft skin filling with blood and the crushed bone around his eye and cheek. He ended up having emergency brain surgery. Coincidentally, they also found and removed a tumor while operating. He recovered to skate another day, and hopefully will remember his helmet.
32. Hearing Voices
Psychiatrist here. One of my first patients was a female college student who couldn't sleep because of the voices that constantly talked to her. Apparently, she felt forced to answer them at all times. From what she was saying, I gathered that depending on the particular voice, she was either being cautioned about people or situations or outright pushed towards violent acts.
The voices started appearing when she was 16 if I remember correctly, and we met when she was 20. For four years of her life she believed that it was normal to have such voices in one's head, because, as she explained, many people talk to themselves. To some extent, she was right; but I had to explain to her that most people really talk with themselves and there are no other identities in them.
There’s just an internal dialogue to clarify or resolve issues that bother them in their own privacy, so to speak. She was later diagnosed with schizophrenia.
33. Not Quite A Baby...
Nurse here. We had a 67-year-old woman who thought she was pregnant. I've got to say, she did look pregnant since her abdomen was full; similar to those pregnant women who look like they're carrying a basketball when they are at the end. But she was 67. Turned out, it was a 37-pound ovarian cyst, and it was the largest one I had ever seen in my career.
I asked if I could watch the surgery. That thing came out all in one piece, and I'll never forget the sound it made. This was at a community hospital many years ago, before HIPAA, so naturally, the lab announced that anyone who wanted could come down to the lab and view this incredible thing before it was dissected by pathology.
The line at lunchtime was so long you'd think they were giving away free concert tickets.
34. A Life Spared
My psychiatrist saved my life! I have always had heavy and irregular periods, so when I had bleeding that didn't go away for a month, I pretty much just kept on keeping on. Eventually, a doctor referred me to the emergency department because of the constant blood loss, and all I was told was "You've got endometriosis". So for five months, I had a heavy period, with doctors just dismissing it.
Eventually, my roommate called an ambulance when I passed out in the shower. The doctors did a blood test and I was admitted overnight for a blood transfusion. Fun fact—blood transfusions make some people nauseous, which is not a fun way to find out you're allergic to an antiemetic! A few weeks later, at about the six-month mark, I drove for an hour for my regular appointment with my psychiatrist.
He took one look at me and freaked out. He told me to proceed directly to the ER. So I did and was promptly admitted to the ICU with a bilateral pulmonary embolism. I was hours away from suffocating to my end. Turns out, all the birth control that the original doctors had been giving me to shut me up and get rid of me had caused massive clots.
The doctor that looked after me and ultimately saved my life wrote a paper on why it's stupid to ignore a nulligravida (never pregnant) woman in her mid-20s with severe dysfunctional uterine bleeding.
 Pexels
Pexels
35. How Incompetent
I had all the symptoms of a GI bleed, including vomiting blood that looked like coffee grounds. I went to the ER, had an NG tube put in, and spent the night in the ICU. They scoped me the next day and determined I had three minor erosions, then they released me with a script for antacids. I thought I would be okay from there, but I felt awful for the next two weeks.
I was tired, weak, and dizzy, but I dismissed it all because it was "just three minor erosions". Two weeks later, my doctor sent me in to have my blood drawn. My hemoglobin was at 4.6 and my hematocrit was 15.1, which is critically low...like "How are you still standing" low. Long story short, I was rescoped at this new hospital and they found a two-inch tumor in my stomach.
It was a very rare tumor that usually doesn't happen to people under 40, and I'm 33. I had a total of five tumors and half of my stomach removed a few days later. Where my GI found the "erosions" was basically right where my two-inch tumor was. I don't get how he missed it, but he found what he was looking for, and that was that I guess.
All I know is I'm not paying the $7,200 bucks that the hospital wants from me. How they missed a two-inch mass baffles my mind. I'm still waiting on the bill for the week-long stay and the surgery in the second hospital.
36. Fancy Seeing You Here
My patient came in with a badly infected foot abscess. Like, the entire foot was showing signs of cellulitis and we had to put her on antibiotics for a few days of inpatient care. She was paying out of pocket and kept trying to leave, but we insisted she finish the treatment. When the infection was mostly cleared she was discharged.
She had strict instructions to change the bandages, monitor the wound, keep it clean, and also had a list of prescriptions. We also scheduled appointments at a wound clinic to monitor the abscess. She did none of those things. She never even picked up the antibiotics from the pharmacy. She skipped her wound clinic appointments and was unreachable.
We later found out this was because she went on vacation. Several days after getting home, she decided to go on a two-week-long camping and river rafting trip with some friends. Her camping trip was cut short after the first week because she developed septicemia and her friends drove her to a local hospital to get airlifted back to our hospital.
37. The Girl On The Grill
The year I was a medical intern I had a 34-year-old woman for a patient. She was manning a grill for two days during a weekend festival for her church. During the festival, her eyes got irritated from the smoke off the grill so she asked a friend for eye drops. After using them for two days, she developed a rash. The rash rapidly progressed to cover her whole body.
It then developed into Toxic Epidermal Necrolysis Syndrome, which essentially means the most superficial layer of the skin separates from the deeper layers. This leaves a wound that is similar to the raw spot underneath a big blister. In her case, it involved three-quarters of her body. Her body was also fighting off infection in her mouth, esophagus, stomach, and intestines.
We had silver-impregnated dressings that we had to wrap her in like a mummy and change every day. Despite everything we could do at the main burn unit in a huge metro hospital, her body couldn’t continue to fight. Her friend was racked with guilt. All over some eye drops.
38. Till Burns Tear Us Apart
I had a husband and wife brought in at the same time, both with major flame burns. He was about half his body surface area, and she was 75% or more. The woman was intubated at the original emergency room they went to. She was waking up a bit when she got to our unit and kept trying to mouth something around her breathing tube.
In hindsight, I'm pretty sure it was "my baby," as she miscarried about 36 hours after she was admitted. She developed an arrhythmia while we were starting a new IV and we couldn't control it. Then we found out what really happened. We found out the husband lit her on fire when he discovered he wasn’t the baby’s father. He survived and after medical treatment moved to a penitentiary.
39. Little Red Dots
When I was about 16, I started having these little red irritated spots show up on my arm. My mom was immediately like, "You have psoriasis, just go tanning". So I tanned for about a week and they just got worse. Now I had them all over my body. I even had spots on my eyelids. I went to the doctor finally, and he made a gruesome discovery.
It turned out I had ringworm. Even worse? By tanning, I was basically rubbing them all over with the lotions and incubating them while I tanned.
40. Never Ignore The Symptoms
My pregnancy was really painful. I was the only woman in my family besides my mother who went through this, and even she didn't get sick at all while pregnant. I thought it was normal that I couldn’t stand straight or go farther than ten feet from the bathroom, or that I spent days on the bathroom floor unable to keep anything down to the point where I would lose track of days.
My fiancé begged and begged for me to go to the ER because of all the pain I had. It turns out, I had an acute UTI that was ready to spread to my kidneys. They told me if I waited any longer, I would have miscarried. The thought definitely makes me hold my baby tighter.
41. A Downhill Spiral
I was the patient. I had a Roux-en-Y gastric bypass in April of 2017. After I went home from the surgery, the expectation was that I would be on a liquid diet for a week, and then slowly start reintroducing soft foods, etc. I even used a check-in app that reviewed how I was feeling, just to monitor if something was wrong.
Two weeks in and I still couldn’t keep down an ounce of protein shake. My husband at the time was getting frustrated with me because he thought I was being deliberately difficult. While he was gone to a city three hours away by plane, I woke up in the middle of the night heaving and dry vomiting. My mother drove me to the hospital in the middle of the night where I spent the next 12 hours having every test imaginable run on me. That’s when doctors made a gruesome discovery.
It turns out, within 24 hours after my surgery, my intestine that was reconnected at the “Y” junction had actually come apart (it was leaking anastomosis, if you want to look it up). Everything I’d tried to eat had just been draining into my abdominal cavity. I was septic and had four large abscesses. After emergency surgery, I spent 10 days in the ICU recovering before I went home.
The surgeon told my mother that if I’d been even 24 hours late getting to the hospital, I wouldn’t have made it. Side note: less than two months later, my husband left me.
 Unsplash
Unsplash
42. That's A Good Call
One time, I got food poisoning. I'd never had serious food poisoning before, but my boss who I was at a conference with had. After clearing myself completely in a very short period of time, I told her I would probably miss the next day. She asked if I needed anything and I said, "No-no... I'm just trying to drink water but I can't keep it down...I've put all my pillows on the bathroom floor so I can stay close to the toilet".
She brought me ginger tea and asked if they could take me to the hospital. I declined and tried the tea which also came back up. After a while, I was still heaving and I could hardly get up, so I finally let her and a co-worker drive me to the hospital. But I felt so stupid—who goes to the ER for food poisoning? They stabilized me in the ER after a few hours and ran some tests.
They told me then I could go home if I wanted, or stay the night in the hospital if I preferred. I'm really not the type to worry about my health and I always assume things will be fine, but some instinct told me to stay. I felt terrible when they wheeled me over to the hospital and I told them that. The next thing I knew, I was on a hospital bed surrounded by med staff. I had a life-threatening seizure.
 Pexels
Pexels
43. Where’s The Horsehoe?
When I was a medical student on my surgery rotation, I was working a shift with the trauma team. I'm observing a simple repair surgery when my trauma pager goes off. I run into the trauma bay and a young gentleman is brought in on a stretcher with the lower half of his body covered in blood, but he's awake and coherent.
He's screaming and had been shot 15 times, all below the belt, and one shot had gone straight through his scrotum. We're doing an evaluation when a code is called in the next pod over. Turns out it’s the patient who was brought in with our current patient. Several of us run from patient one and into the next pod to see a woman lying on a stretcher receiving CPR.
We roll the patient on her side to get her clothes off and notice she's bleeding out of her back. There is a tiny exit wound and we piece together it’s a ricochet from our previous patient. We take her to the trauma bay to perform the primary surgery. She's not breathing and has no pulse. We intubate and find the entry point in the center of her chest.
Ultrasound confirms a hemothorax and we get a chest tube in place. Instantly there are two liters of blood gushing onto the floor. The resident I'm with immediately takes a scalpel and makes an incision, then they clip the sternum in half. This woman’s chest is now completely open and we can see the heart, and the clean entry and exit wound.
All of the blood and fluids we were pushing was just draining right out of her heart and into her chest. We’re running her to an OR, when I notice she’s bleeding from every single opening in her body. Her body had used all its clotting agents. The blood still flows but she can’t go for surgery under this duress. We transfer her to intensive care and monitor her for three weeks.
She can't talk or move, and the family is having conversations about life support. I find out she was discharged as a quadriplegic and the future is bleak. The real twist happens six months later. I was working a shift in intensive care and bring up this patient to my attending. They remember the night and working on the body and proceed to tell me that a month ago at a follow-up visit, this patient walked in. After the awful experience, all she has is a scar from her thoracotomy.
44. Going Great Lengths To Stay Hip
Our elderly patient went into cardiac arrest but was revived. We did all the possible tests but couldn’t find the reason. Just as she was getting better, her heart attack came back for a sequel. We did CPR and were able to get her pulse back, and closely monitored her that night. Things were not looking good so we called her husband.
We asked him to come in as we were worried she would not survive the day. Her husband told us he would be there within the hour. Well, three hours passed and he didn’t show up. We tried calling and couldn’t reach him. Eventually, a nurse found out that he was downstairs in our ER! Apparently, when he left his house in a hurry, he fell and broke his hip.
45. A Medical Mystery
A patient mystery I never understood was a healthy 23-year-old male. He came into the ER with chest pain that started after eating something spicy. We check his vitals, do an X-ray, and are about to discharge him when he collapses lifeless. We start CPR and get a pulse. He was stable for a CT scan but doesn’t survive the procedure.
The team was baffled. During the autopsy, it was revealed his major blood vessels basically just imploded. This sometimes, though rarely, happens to men in their 70s with a long history of lighting up and high blood pressure, but this patient had zero risk factors and was a non-smoker. This was a few years ago but the case still bothers me.
46. Fix One Problem, Find Another
My sister was having stomach surgery and the surgeon mentioned that her uterus looked strange. The surgeon thought there might be an ovarian cyst and recommended getting checked. After she recovers from the stomach surgery, she checks out the uterus, and she finds out she has uterine leiomyosarcoma. In other words, her entire uterus was just one big tumor.
The tumor also impacted her ovaries and her fallopian tubes. She had another surgery where they got it all out and then she went through chemo for five months. After six months of clean scans, she goes to get a mammogram and finds breast cancer. She chose to have a mastectomy last week and she starts radiation soon. It’s the worst treasure hunt ever.
47. A Clot Unlike Any Other
My father went to the hospital with chest pains, and they decided to do an angiogram. The process injects dye into his valves to look for clots. During his procedure, the surgeon asks if he suffers from blackouts, and a few more doctors get called in to have a look. My dad is the strong silent type but admits to minimal daily pain.
They take him to another type of X-ray machine and again are looking in bemusement without explaining anything. Turns out there was a blood clot the size of a golf ball floating free in his heart. It normally should have taken out someone quickly and the doctors were all intrigued. He had a triple bypass 30 years ago and is still the strong and silent type.
48. A Mumbling Clue
When I was a fourth-year resident, my first rotation in the hospital was in radiology. I was waiting with a patient after an ultrasound and they told me they were thirsty. They take a sip of water but then start mumbling. It was incoherent to us but his daughter said he had spoken like that before. She said something felt off. She was all too right.
One second he was fine, and moments later he’s just quietly staring off into space and I start to wonder what’s going on. We check him and one of my seniors calls our resident and immediately starts CPR. He was wheeled down to the ER but we lost him later that day. Since then I’ve had many patients but this memory still makes me feel weird.
49. More Than Just A Headache
I've always had headaches, almost daily. About 10 years ago, I started seeing weird auras that would take up my whole vision, and then I'd get a terrible headache that would make me want to end it all. Maybe once a year that would happen. About three years ago, we got really good insurance. Then, I got several auras in a row, and I started to worry that it was a detached retina or something.
So I went to an ophthalmologist, who dilated my eyes and looked around. He suggested I see a neurologist, and maybe they'd do an MRI. Meanwhile, I had a stomach ache that lasted for a few days—very odd for me, since I don't really get them. But it woke me up in the middle of the night, and I had another aura visual—but no headache.
I saw the neurologist a week later and boy did he like talking about how fat I was. I had three kids in three years, so naturally, I became squishy—not morbidly obese, but I did have some mobility issues. Deal with it. They were able to get me in for the MRI that day, and despite being claustrophobic, it wasn't terrible.
I walked out to the parking lot, and they called me back in. When I got in, she told me I'd had a stroke, and they needed to admit me to the ER. The office was at the hospital already, so she literally just walked me through like two doors, and I didn't even have to wait in the lobby. I spent three days being poked and prodded.
I never really saw the big deal, it was just a stomach ache and dancing lights. I'm doing a lot better now.
 Pexels
Pexels
50. Painless Yet Severe
When I was 14 years old, I started getting an upset stomach one night and it wasn't just another bellyache. Maybe a little bit more intense, but I slept through it pretty well. The next morning, my parents got me an appointment with the doctor to see if I was okay. We got through it all, but we had to wait at one point, and it was taking quite a long time.
I told my mom, "We should just go home, it's probably nothing..." and then the next thing I knew, I needed surgery. When I was talking to the doctor before the surgery, he explained that my appendix had burst, and he said I just had a very high tolerance to pain. In fact, he was surprised I was able to sleep through it.
He also explained that if I didn't have surgery when I did, I wouldn't have made it. I can see now why a lot of people think that having a high tolerance to pain isn't necessarily a good thing.
 Pexels
Pexels
51. One Exam Is All It Took
I had been suffering from debilitating pain basically since I was 14 years old. They were worse around my periods and would kind of dull down afterward. I was told this was “normal". When I turned 18, I started searching for answers because the pain was getting worse. I went to seven different doctors in six years. It was constantly being dismissed as “normal” period pains.
One doctor even tried to tell me it was irritable bladder syndrome. I was no medical student, but even I knew that was not a real diagnosis. I was on all kinds of different birth control and pain medications which did not help. At 23, I was finally able to see an OB-GYN who specializes in pelvic pain. She barely even touched me before she was saying, “Oh my! You have endometriosis".
She scheduled me for my first laparoscopic surgery in January. During that surgery, not only did they find that I had the highest and rarest severity of endometriosis with complications, but they also removed several golf-ball-sized cysts that were ready to rupture. She told me I must have a really high pain tolerance because I should not have been able to walk upright into her office that day with everything that they found and removed.
The most amusing part of it all was that before seeing the specialist, I had three ultrasounds and several other exams, but none of them detected or even bothered to look for endometriosis or PCOS. It was that simple pelvic exam that saved my life.
52. Simply Counterproductive
Nurse here. At a get-together with friends (where the drinking got out of hand), I had a friend burn himself in the oven while making pizza, then try to cauterize that burn with his lighter. Fun fact: you cauterize wounds, not burns.
 Unsplash
Unsplash
53. Quack Medicine
I'm a pediatric nurse. This one couple brought their child and he was feeling really weak. After the general admission questions, we discovered that they were into natural treatments. When their infant child developed tummy problems, they decided to give her a bottle of honey water to help with that. The baby was diagnosed with botulism.
54. A Tickle In The Throat
In my first year as a nurse working in oncology, we had this cute old man who had esophageal cancer. He had a golf ball-sized mass in his throat, and he had gone through radiation treatment but his doctor decided he needed a tracheotomy. Just in case you don't know, this procedure cuts a hole near your Adam's apple to form an airway.
His procedure never healed properly and the patient was constantly in pain at the surgical site with excessive ooze and liquid, I’m talking cups every hour or two. This wasn’t normal but it wasn’t impacting his airway, which was the most important thing. We continued to monitor the patient carefully through his radiation treatment.
We would suction out the liquid every night but one night, the suction started pumping out blood. I’m trying to stay calm and thought he’d gotten scraped when they changed the inner cannula of the trach recently, but then it got worse and worse. All of a sudden, he coughs, and his bleeding trach turns into a literal faucet of blood.
My suctioning can’t keep up with the blood flow and it starts to flow into his throat, and is choking him. I’m yelling for help as blood is pouring down his chest and all over my arms. Eventually, with CPR he was unresponsive and we couldn’t get a pulse. In the end, we presume the trach had been irritating the wall of his throat, and the radiation was making it worse.
55. Twice The Fun
My mom is 4’11”, so when she was pregnant with twins, she was almost wider than she was tall. They had her on bed rest in the hospital because they knew we’d be early. She had gestational diabetes and hadn’t had sugar in months. My loving, caring father was by her side the whole time and had also cut out sugar to support her.
On this specific day, however, he was sneaking a chocolate shake, and my poor mom became really emotional and asked for one sip. Immediately as she took the sip, her water broke. Of course, it was unrelated to the chocolate shake, but my mom was beside herself, thinking she messed up and caused early labor by drinking a chocolate shake. Oh, and there was one more thing.
After a successful delivery, my mom had intense pain. She couldn’t even blink her eyelids, her body was on fire. They rushed her to surgery and had to remove her whole gallbladder, which according to her was worse than childbirth. The constant optimist, my mom was just happy to stay in the hospital longer while we were in natal intensive.
56. Balance Out The Breath
I’m a patient, and I'm just remembering a wild diagnosis. I was 19 years old and started experiencing shortness of breath. It would happen if I exerted myself, like running to the bus or climbing stairs. I decided I was out of shape and made plans to start going to the gym more. That night, however, I got dizzy walking to the kitchen, and I knew it was time for help.
My parents were out of town so I asked my neighbor to drive me. I figured it would be a quick visit and felt a little embarrassed going in the first place. Turns out I had two clots in my lungs, a side effect of my birth control. Full treatment was four days in the hospital, heavy blood thinners, and a wheelchair for a few weeks. Thank God I checked.
57. All In Your Head
In 2014, my sister got rear-ended and suffered from whiplash. She began to get awful headaches, and she'd go to the doctor but they couldn’t find the cause or solution. Over the next year, the headaches got worse, and she started to have problems with her body functions. Sadly, everyone she talked to said it was just in her head and was dismissive.
At the time, she worked for UPS and got hit in the head with a box that was dropped from above, which only made things worse. She then developed problems swallowing, breathing, and began having seizures. In September of 2015, she came to my house after school one day and laid down on my couch, and then didn't get up for months except for the toilet.
One day, she managed to finally convince someone to give her a cervical MRI. At that point, the doctor called me in a panic to come in, but I wasn't able to go with her. She called me in tears later because they had finally found the cause. It turns out the whiplash had made a previously unknown Chiari Malformation symptomatic, and her brain stem had fallen out.
Yes, really. It was compressed against her spinal cord and shoved into her first cervical vertebra. The back of her brain was just hanging out of her skull. She had decompression surgery but suffered irreversible damage due to the length of time she was untreated. Turns out, it wasn't all in her head and her primary care doctor had never even heard of Chiari Malformation.
58. A Puddle Problem
I was working in the ICU one night, and it was fairly quiet. I had this older gentleman, in his 60s, admitted with hepatitis. He started complaining of pain in his stomach and chest so I gave him some morphine as he was prescribed. A short time later, I asked him how the pain was. He looked visibly uncomfortable and stated it wasn't any better.
He started moaning and pleading for help. I called the resident and got a further order for morphine. A short while later, he's calling me over and is now pale and restless, stating the pain was worse and begging me for help. I'll never forget his moaning and pleading. My nursing intuition knew something wasn't right. I turned around and walked to the phone.
I called the resident again when suddenly I become aware of a dark shadow growing and spreading under the patient’s bed. There was no mistaking this dark red puddle growing rapidly. I Interrupted the resident and said "you need to get here right now" and hung up. I ran back over to the bed and confirmed that the puddle was his blood.
Before I had the chance to say or do anything, the patient suddenly threw his head back and passed out. He went very pale and then blood spurted out of his mouth. In fact, it seemed like blood was coming out of every orifice. It was spurting, like a waterfall. I'd never seen so much blood. By the time the resident came running in the door, the patient was gone.
59. Elastic Heart
A patient came into the ER presenting with very serious heart pain that caused him to pass out frequently, sometimes daily. Apparently, he just thought it was because he was overweight. We had to explain that passing out for no reason is not normal and that he should have told his doctor about it. The problem itself was sort of on and off, so initially, we didn't know what was up because his vitals all looked good.
When none of the meds we gave to him helped, we ended up sending him to the hospital. His heart rate was dangerously high for a pretty sustained period of time (like 45 to 60 minutes), so he started passing out due to a lack of oxygen. Turns out, he had been suffering from minor heart attacks, not realizing how serious they actually were—but that’s not the worst part.
This had been happening to him since he was at least a teen, if not younger, and his parents never thought to bring him to a doctor about it.
60. A Nasty Fall
I came off my bike during lunch break at a real slow, walking pace after the wheel jammed on a gutter. I went over the bars and had a nasty landing. My right wrist swelled up almost instantly, so I isolated it, thinking it was a probable Colles’ fracture. Then, I proceeded to walk the 1.5 km back to the office in cleats; that is, carbon fiber shoes that have no flex in the soles. I had to push the bike too.
I was in a lot of pain, so I went to the hospital for scans. The triage nurse assessed me and came to the same conclusion I did. I was given an ice pack while waiting for the doctor to look at the X-rays. I was in tears the entire time the films were being done and I don’t normally cry either. The only comfort from the radiology tech was “There’s a reason why you’re crying, but I’ll leave that to the doctor".
It turns out, I had sustained bilateral radial head fractures and a broken left wrist. The swelling in my right lower forearm was a reaction to the broken radial head. I spent eight weeks in akimbo slings plus three months of occupational therapy to teach my biceps how to bend my arms again. Nowadays, I only have 90% bone strength in those joints.
 Unsplash
Unsplash
61. And Just Like That...
My father felt a loud pop as I was helping him out of bed. This wasn't unusual and my father thought he just pulled something. However, the pain didn't subside for weeks. I dragged him to the GP, and then to the hospital for a scan. The “pop” turned out to be the back of his rib totally separating, as the bone was mostly powder—and the reason why was awful.
He developed lung cancer from his bad habits as a young adult and it had grown through the back of his lung and into his ribs and spine. He was in palliative care from then on. At least he got to say goodbye to his cat Tilly—I brought her into the hospital and he let her loaf on his chest with her bum in his face for one last time.
62. Will It Ever End?
My best friend was the patient. She was diagnosed with a hernia and was set to have surgery a year later because it wasn’t so bad that she needed to have emergency surgery. Eventually, she decided to go to her home country, because she felt she was being mistreated by the health care workers in her US town. She was scheduled to have a pre-surgery check-up, and then the surgery two weeks later.
Well, when she went for the check-up, she got taken to the table without anesthesia. While she was being operated on, she could see what was happening, which was frightening enough. Then, they uncovered the root of the problem—she had a birth defect that ended up causing a massive cyst to grow. She was in great danger. She had trouble walking and had to take a flight back the day after.
She is doing much better now, but she recently got diagnosed with another hernia on the other side.
63. Secondary Complication
In my freshman year of college, I had a really bad sore throat for a few days. I thought nothing of it and just took a ton of Tylenol until it went away. About a month later, I noticed the joints in my fingers were extremely sore and I could barely make a fist. Next, it was my wrists, elbows, knees, ankles, etc. It reached all my joints and muscles.
It was even painful to lift my eyebrows or touch my scalp. I couldn’t roll over in bed. I literally just lied in bed for days and cried. Finally, my mom, who lived about four hours away, came and took me to the doctor. I couldn’t believe the diagnosis. He said I had something called post-streptococcal arthritis. Turns out, I had strep throat a month prior and because I didn’t treat it with antibiotics, it spread through my body and caused arthritis in literally all of my joints. He prescribed a steroid and pain killers and said good luck!
Man, I’ve had a lot of medical problems in my life but this one was the worst by far. It took another three months for me to start feeling normal again and a full year to get completely back to normal. Nowadays, I catch strep throat extremely easily and I get it at least four to five times a year. If I don’t get it treated within two days, my arthritis flares back up again.
64. An Ax To Grind
My stepmother was a general practitioner but got to spend some time in the ER and EMT services during her studies. One night in the ER, a woman walks in...with an ax stuck in the middle of her head. Apparently, the ax had done no damage and the blade was simply embedded in her head. As it happened, her husband had taken a swing at her during an argument.
She never told me what the argument was about but she survived and made her way to the hospital. She had to drive herself with the ax's handle dangling in front of her face. It was impressive, to say the least. The good news: she divorced her husband!
65. A Rollercoaster Of Emotions
On my last day at my previous hospital, we had a patient with chest pain and low blood pressure. He'd had no symptoms prior to passing out at home. We get him hooked up on the monitor, get an electrocardiogram and an IV, and noticed his results looked funky, like he might have a heart condition. Nonetheless, his history is clear of it.
We go to the doctor, who says to run the test again in 10 minutes. The second test had different results so we run a third, which also produces different results. The cardiologist is now convinced that we had mixed up his chart with someone else's. He's sitting there with 6/10 chest pain and results that looked like they were all from different people.
Suddenly he passes out and we can’t find a pulse. We start CPR and revive him. When he wakes up he’s yelling and angry at everyone around. We're getting him prepped for a CT scan but his blood pressure is unstable. On the monitor, we see an abnormal heart rhythm, but he’s laying back and talking to us. Then we can't find a pulse.
The monitor now shows he’s in cardiac arrest but he’s still awake and answering questions coherently, even though we still couldn’t find a pulse. When he loses consciousness, we do CPR and shock him back. We decide to move ahead with the CT scan. He passes out in the machine and we are again giving him CPR. Each time we repeat this and shock him back.
We go through this a total of 19 times. I’ve still never seen someone get shocked that much since. We couldn't tell when we needed to start CPR if he wasn't talking to us, so I had to stay bedside. We eventually found out his aorta was riddled with clots. He got up to ICU and was a total nightmare of a patient. Hostile and grumpy the entire time, but somehow managed to survive and get discharged.
Everyone involved with that guy celebrated after work the day he left. The whole experience was tough and a rollercoaster for everyone that met him, since we never knew what to expect.
66. Resident Roulette
When I was in residency, we had a patient that came in for a quick visit to test their leg circulation. We run the test and there’s trouble getting a reading in his left ankle. We try again, and still no reading. We’re all checking the equipment, and one resident takes off his sock. We were shocked at what we saw. The sole of his foot was totally black.
One of the other residents squeezes his foot and their thumb sinks into the flesh. When they pull their thumb out, a cup full of grey liquid flesh starts leaking out. I think I’m going to be sick and one resident almost passes out. Thankfully, a nurse rushes over and tells us to get him to vascular. The simple test discovered necrotizing fasciitis and turned into a below-the-knee amputation that night.
67. May The Floss Be With You
I’m a dentist, and had a young patient who came in for an evaluation with complaints of tooth pain on an upper molar. We take an X-ray, and the molar has a large cavity that has reached the pulp tissue of the tooth. This is where the nerve sits, and the infection has created an abscess. The patient’s options were a root canal or pulling out the tooth.
The patient didn't show too much interest in either option and left the office with an antibiotic prescription. Flash forward to six months later, and I see the front desk has an emergency patient in my schedule. The description says the patient is in severe pain and can’t talk at all. I figure it’s another dental abscess patient with a rotten tooth.
I come into the room and realize it’s the same patient that I saw six months ago, but this time he is with his partner. The patient clearly can’t communicate, so his partner is telling me about the severe pain, plus trouble talking, eating, and breathing for the last three days. We can’t take an X-ray because he can’t open his mouth, but we try a panoramic X-ray.
Well, the same tooth from six months ago with the infection has escalated. I take a look inside and see that the floor of his mouth is raised significantly, and it's also as hard as a rock. I turn to his partner and say they need to go to the hospital ASAP. I phone an oral surgeon colleague and explain to him what I see.
The patient goes to the oral surgeon’s office before the hospital, and the surgeon calls me after the examination. It was worse than he anticipated and the patient was on the way to the hospital pronto. The patient needed to be in the hospital for five days before the successful surgery. Don’t underestimate a simple toothache.
.
68. With Friends Like These...
I’m a paramedic and a few years back, I worked for an ambulance service that included an area home to a summer nudist colony. We would be called every few days for minor falls or people with colds or flu. This call came in at 9:00 pm and said the patient at the nudist colony was fainting. We head over and are introduced to the patient.
He’s in his 80s and was visiting from Poland. He's sitting at a campfire, enjoying a few drinks with his equally unclothed friends. His wife said she called because he kept passing out after complaining of heartburn. He said he's fine and was just tired from the days’ festivities. All in all, pretty lighthearted scene, but he didn't want to go to the hospital.
I convince him to let us do an EKG before we leave and it shows that he’s having a heart attack. I run the test once more and then sit down next to him to deliver the news. The mood changes and the group is now begging him to go to the hospital. He concedes, hugs his friends, and gets in the ambulance. En route, we do our routine cardiac care.
A week later, we get called out to the nudist colony again and arrive to find we're treating the previous patient’s wife. She was now having heart problems which was luckily just a case of angina and wasn't very critical. Our patient from before is there, and said the doctor told him “the ticker is good, I just need to be careful getting excited around all of my friends".
69. First Day Jitters
This was my first day of surgery rotation while I was still in medical school. Our patient was a middle-aged woman. She was unconscious, pale, and possibly bleeding internally due to self-inflicted wounds in her abdomen. There were multiple cuts and we found out she did them after finding out about her husband’s infidelity.
We immediately went into surgery to locate the source of internal bleeding. After a few moments, we were able to stabilize her and checked every segment of her intestines for bleeding. There was one that missed a major artery by millimeters. As we were preparing to close up, my chief resident decided to take one more look. It all ended in horror.
While doing this, he accidentally caused a big artery to bleed. We had to call the chief surgeon, even though he was on vacation. He answered and was calm while telling us what to do via the phone. We were able to control the bleeding by a combination of aggressive cautery and some pressure plus suturing. The patient spoke to me a few days later as she recovered in the ICU bed.
70. Get It Off My Chest
A 40-year-old woman, who was a successful business owner and fully insured, had been taken to the ER by her sister because she was complaining of chest pain. She was asked to put on a gown for an EKG. I will never forget the sight. Her skin literally looked like a green hamburger. Sadly, she did not seek care sooner because she said she was embarrassed by the appearance and odor.
I followed her care as best I could. She went through a bilateral mastectomy, radiation, and chemo. She survived another three months before she passed on.
71. Beyond A Burp
I had been having a problem for about two months where I'd feel some pain or pressure in my chest, specifically in my left lung. If I bounced a bit or tried to take a deep breath, I would normally need to burp which made the pain disappear, so I always thought that I had just swallowed some air or something had gone down the wrong pipe or whatever. No big deal, I thought. I was so wrong.
Over time, it got worse and worse. I would burp more, and once or twice per week, I would have a splitting pain which made me unable to turn on my left side. I also couldn't sleep at all and was just tossing and turning most nights. I had waited a total of 23 hours from when the pain first started to when I notified my mom "I might have to go to the ER".
Turns out, I had a collapsed lung—not partially deflated, but completely collapsed. It was bad enough that it was pressing up against my heart and disrupting its rhythm. Two operations later, I was okay, and through the glory of healthcare, the total hospital bill I had to pay was only $25.
72. A Hero's Weakness
I have what’s called Haglund's deformities in both of my feet. Essentially, I have bones growing from the back of my heels through my Achilles' tendons. Every time I walked or ran, it would rip and tear a bit more, forming scar tissue called a bursa. I would only feel the pain after I had finished running, and the only time I was running was when I was playing rugby.
I had this for close to 20 years. I always thought it was normal as I never really looked at anyone else’s feet in great detail. When I tore all the ligaments in my knee, the doctor saw the lumps and told me that the only way to get rid of them would be to cut through my Achilles, grind the bone away, and then reattach my Achilles. As I would have to learn to walk again, I essentially just chose to stop playing rugby...
73. Necrotic Neglect
My mom is an RN and she was just telling us about this lady she met while working in the ER a few years ago. This lady was morbidly overweight, diabetic, and bed-bound. She called 9-1-1 because she was worried about a smell coming from her bottom half (again, she was morbidly obese and could not bend over far enough to see what was going on).
She got seen by a doctor who checked her feet out. The doctor apparently said they were as black as a chalkboard, which was going to result in her losing her feet. When the doctor asked why she didn’t have anyone checking in on her, she said she never thought to bring it up to her kids as she thought the tingling and diabetic pain was normal.
74. Aging Too Fast
I remember saying once in college that if my hands hurt this much now, I’m going to end myself when I develop arthritis. It turned out, I already had it. I was recently diagnosed with rheumatoid arthritis and hypermobility. The hypermobility is not as severe as EDS, but it’s notable. Just this year, I’ve dislocated a couple of fingers, my wrist a few times, and both kneecaps.
One was a full dislocation that had me on crutches for a few weeks and constantly subluxated. My doctor thinks the inflammation is newer, but that I’ve been dislocating my joints for years. I genuinely thought everyone was in as much constant pain as I was, and that they just managed it better and coped more efficiently.
75. Forget About It
I have a ridiculously high pain tolerance. The joke goes that I might lose a couple of limbs and it will take me a while to notice. I had some minor pain around my lower stomach and back. I didn't think of it much—I assumed it was some minor GI issue. I took paracetamol and honestly forgot about it. This went on for several days.
Later that week, I suddenly started feeling seriously ill. Cold sweats, chills, fainting... I thought I might have somehow messed up the medications or something. In the ER, it took just a couple of tests to figure out I had a severe kidney infection, and considering the severity, it had been going on for at least a month. I only felt minor discomfort for the last few days of it.
76. One Wild Night
Last October, after a wild night, I fell into some bushes by the side of the road. I'd drank a little too much, though I always wonder if I'd been pushed. Anyway, it wouldn't be so bad except for some reason, the sidewalk I'd been on was elevated by about 1/2 meter from the base of the bushes. There was a concrete patch (which I later discovered to be a manhole) right where I landed on my right shoulder.
I got up, checked that I had full hand and finger mobility, and if I could bend my elbows. I couldn't lift my arm above my head without some pain, but I figured I should be fine. I cleaned myself up, got home, and went on with life as normal. The next two days it was a bit rough trying to lift my right arm, but after that, it was more or less okay. I dismissed it as a muscle strain.
10 days later, I picked up my daughter and felt a searing pain in the shoulder where I had fallen. It still wasn't so bad, but since it hadn't gone away after 10 days, I thought I should probably get an X-ray done. I had actually gone to see a doctor who asked me to get one done, but it slipped my mind. So fast forward to the X-ray scan—and I heard what you never want to hear. The X-ray technician exclaimed, "Oh!'" right after the first one.
Then, I heard a muted phone call between him and the doctor I had seen earlier that day. When I was dressed and came out, the X-ray technician told me he couldn't believe I'd been walking around for 12 days without pain. My clavicle and collarbone were broken. On the right side, the bone was kind of tilted upwards, and it was totally separated from the left.
By the time I got surgery to get the collarbone fixed, almost four weeks had passed since I fell.
77. Not The Face We Were Expecting
I worked in a rural area of our county and treated a self-inflicted wound to the head. Unfortunately, this happens a lot, and we have to show up to “pronounce” them deceased for law enforcement. As a paramedic, we’ll also play mini therapist for anyone who was there because that’s something that’ll mess with you no matter who you are.
Prior to showing up, though, we always park a ways away, waiting for law enforcement to enter the scene. As we’re waiting we get an update that a female witness has passed out and become a second patient. Dispatch gets a second ambulance en route and luckily they weren’t far away. Finally, dispatch calls us and says we’re cleared to enter the scene.
Our dispatch team also says law enforcement is requesting lights and sirens, which is an odd request. Normally they just ask us to proceed, but we also have to manage public perception. We assume they know something we don’t and comply with the request. The second ambulance comes from a different direction and beats us by 30 seconds.
We park right behind them and hop out. My partner checks if the second ambulance needs anything while I go assess the second patient. I see a distraught younger female sitting in the grass and she’s screaming and crying uncontrollably. I then hear my radio go off “patient one in critical condition". I glance at the front door and see them walking and sitting on the stretcher.
I get in the back of the second ambulance and set up the equipment they’re going to need. I set up an IV line, grab a bag with intubation equipment and a medication box that has pain and sedation stocked. We load the stretchers in backward and the first patient is sitting up moving around. I thought this was a good sign—how wrong I was.
The first patient had chosen the wrong angle and they basically had no face to speak of, but they were still breathing. What I remember most was just every time someone walked by our ambulance, they just stopped functioning and stared. It didn’t make any sense that he was alive. We performed a surgical cut for him to breathe, and he was flown to a trauma center.
78. One Foot Forward
When I was a paramedic, we responded to a call from a man in his late 40s who lived with his invalid mother in the middle of the country. He wanted us to check his high blood sugar levels. When we ran the numbers, they were the highest my partner or I had ever seen. We advised him to go to the hospital immediately; he was morbidly obese and wasn't taking care of his type II diabetes.
He refused our attempts to admit him and drive him to the hospital. We can’t force him into the ambulance and had no choice but to leave him. As soon as we could, we advised our medical control of the incident. The second phone call came two weeks later. With this gap in treatment, his feet now have gangrene and we can see the exposed bones of his toes.
I mean all 10 of his toes have had the soft tissue eaten away and are down to the bone. This time he wasn't the least bit hesitant, but I still can't believe he waited for it to get as bad as it did.
79. Savior Sibling
When I was a resident, we cared for a toddler admitted to the ward with a newly diagnosed tumor. Her mom had just delivered her baby sister at the adult hospital across the street three days ago. Due to nursing, baby sister is allowed to stay in big sister’s hospital room. The nurses call in the middle of the night because baby sister “doesn’t look right".
When we arrive she is blue, poorly responsive, and breathing hard. We take the newborn to the emergency room downstairs where she is promptly intubated, resuscitated, and diagnosed with a cyanotic heart lesion. Within an hour she’s undergoing successful open-heart surgery. She owes her sister for the save since they were already in the children’s hospital when she deteriorated.
80. Rival Redemption
I was an intern in the trauma surgery rotation. In my first week, we have a known gang member brought in by private car. No one stayed with him and he crawled into the ambulance bay for help. There were multiple gunshot wounds to his chest and abdomen. He was bleeding from everywhere, and he needed immediate surgery.
We needed to locate entry wounds, deal with a collapsed lung, and keep him from bleeding out. In the midst of this controlled chaos, pandemonium breaks loose. We find out an armed man has entered the hospital. We go into lockdown and believe it’s a rival gang there to finish the job. They were asking about our patient aggressively.
We start erasing the trauma whiteboards that say the patient’s name and injuries and lock down the trauma bay. We cover his face with a drape and can’t go for scans because we are stuck. We are working blind to keep him stable and also unsure of what could come through the doors at any moment. My attending was so calm and set the tone like a champ. In the end, the patient lived, but left as soon as he could stand.
81. Investigative First Response
I’m a paramedic, and we were responding to a road accident. The authorities had detained the driver, and we were checking the passenger in the back of their sedan. We couldn’t see visible damage to the car; it was a fender bender at most. Our passenger, however, was disoriented and resistant to everything. All we could see was a tiny cut on the back of his head.
We struggled to get him out of the car, to check his vitals, and to use a stretcher. Every time he just closed his eyes and pushed us away. We tried asking him what happened to his head and he refused to answer. His behaviors didn’t make sense with the minimal car damage, but we knew we had to get him to the hospital. Later in my shift, I checked in with the team and got shocking news.
Turns out our patient actually had a basilar skull fracture and bilateral subdural hematomas, and we had absolutely no idea how it happened. It taught me to assume there’s a medical cause to any of my patients' conditions, and not to overlook anything. In our roles, we can often miss the big picture, and that can cost lives.
82. Eye Spy
Over the course of about three and a half months, I was treated for a sinus infection six times and then misdiagnosed with migraines—I have a family history of them. I would get these headaches that started in my face and trickle down all the way to the base of my skull. It wasn't until I was referred to an eye doctor, just to make sure that my headaches weren't being caused by my eyes, that the "Oh man, this isn't normal" moment happened.
During a routine eye exam, the doctor discovered that my optic nerves were swollen. She finished her exam, then very carefully explained what it could be. She then made an emergency appointment for an MRI. It turned out that I have intracranial hypertension, which means I make too much spinal fluid, and when it doesn't have any place to go, it can back up into my skull.
Less than a week later, I had to have a spinal tap to drain the excess fluid. I had more than one neurologist's jaw drop when they found out that my pressure level was at 33. The swelling in my optic nerves was so bad that by the time I finally saw the doctor who made the diagnosis, my vision was so screwed up that I couldn't read a book.
My mom had to fill out the paperwork because I couldn't see it well enough to fill it out on my own.
 Unsplash
Unsplash
83. The Childbirth Equivalent
I was diagnosed with acid reflux, not understanding how people dealt with the pain and discomfort. Jump forward a few months—I started dry heaving one morning (after throwing up everything including sips of water) and I decided to go to the ER. One look and they assumed it was gallbladder issues. They gave me some pain meds, but they didn't help much.
Well, an X-ray and CT scan later, it was determined that I had acute pancreatitis. Apparently, the pain is about equivalent to childbirth, or so I was told. A few days later, after pancreatitis resolved, the doctor wanted to send me home for outpatient gallbladder removal. I argued that I was not leaving without the surgery. The next day, they removed my gallbladder in pieces because it had gangrene onset. Had I left the hospital, who knows what could have happened.
 Shutterstock
Shutterstock
84. Luck Of The Draw
I’ll state up front that I’m a rather large girl and have been since I was a kid. I'm always tired and I pretty much get called lazy by anyone who knows me. I can never miss meals or I will get so tired that I would fall asleep on my feet. Growing up, I got told constantly that I was attention-seeking and just needed to lose weight, etc. Well, they were all horribly wrong.
I had multiple blood tests done and they showed I had a slight increase in the size of my red blood cells, but nothing explained why I was so tired. Years later, after noticing some spots appear on my body from my feet to my neck, I started to swell to the size of a balloon. I was told multiple times it was just scabies, so I started peeling off skin in multiple layers right down to the fatty layer.
Later on, the hospital decided that it was a bit more than scabies. Three weeks of pain later, I found out that I had multiple auto-immune diseases. One of them was rooted in a vitamin B12 defect, whereby my antibodies stop the binding of B12 in the stomach, causing pernicious anemia. The reason I am so tired all the time is that my blood cells cannot transport as much oxygen around the body.
I also have a slight gluten sensitivity that was beginning to transform into lactose sensitivity. All my specialists thought my case was very unique. "You’re in your 30s; why was none of this diagnosed as a kid?" Yeah. I wonder why. As for the spots, the doctors at the hospital still have no idea what the heck started that. They just think it’s some variant of a common skin disorder.
 Unsplash
Unsplash
85. Letting It Fester
My mom is a medical assistant in a pediatrics office. About two years ago, a lady came in with a gash in her heel. The lady had thought the tingling was a bad sign and that she should get a check-up...but mind you, the gash had been open for weeks. My mom undid the wrapping the lady put on her foot and there were maggots eating at the lady's flesh inside her foot.
My mom and another medical assistant had to dig them out from this lady's foot. The night she told me this, I was dumbfounded by how stupid this woman was not to go to a doctor once she got the gash.
 Unsplash
Unsplash
86. Saving Money At What Cost?
I had traveled internationally and started having bad stomach problems. I have IBS and assumed my change in diet while traveling triggered the symptoms. I considered going to a doctor but was worried I’d get stuck with a huge bill for a foreign ER visit over probably nothing. I made it through a few more days feeling thoroughly horrible and somehow made it through the two long flights and long car ride home.
Thankfully I had an aisle seat for both flights since I was constantly getting up to use the bathroom. I arrived home on a Sunday evening, and the following Monday was a federal holiday, so my doctor was closed. My insurance charged a lot to go to urgent care, so I figured I’d wait until the following day to go to the doctor. At that point, I was still thinking it might be IBS, but also starting to think it might be food contamination.
When I saw the doctor, she immediately prescribed a strong antibiotic as well as an anti-nausea medication so I could keep it down. I got my test results back a few days later, after I was already feeling better, and discovered I spent a week with E. Coli and campylobacter (another foodborne virus). Had I known how sick I was and how quickly antibiotics would help, I would have gladly paid the premium to see urgent care or even the foreign ER.
 Shutterstock
Shutterstock
87. Love The Skin You're In
I'm an ER doctor and there’s one case I’ll never forget. I had a patient come in for a cast removal literally YEARS after it had been put on. She had just decided it wasn’t worth taking off. Her leg skin was literally growing OVER the top of the cast and then down it. Once we finally cut the cast off, she was surprised to find that she had no skin underneath...
Instead, the dead tissue over her muscles and bones was being cleaned by about 300 maggots. I knew by the smell that something under there wasn’t right, but wasn’t expecting that. The patient seemed completely fine with it. Whatever.
88. A Smell That Lingers
Our patient had severe abdominal pain and we performed an exploratory laparotomy since she couldn’t sit still for a CT scan. Based on an X-ray and the rock-hard feeling of her body, we knew there was fluid building but felt blind to what was going on. When we opened the abdomen of this woman, the entire room instantly smelled like hot garbage.
The smell enveloped the room instantly, and I ran to grab the peppermint oil to rub on our masks. We saw that she was going into multiple organ failure with a ton of tissue simply turning rotten. Our lead surgeon announced this surgery was a mistake, and the patient didn't make it.
89. Exhale For An X-ray
I am an ER nurse, and we had a patient come in with what he thought was bronchitis. He was trying to calm his family down and believed he would be fine in a couple of days. His chest X-ray showed pneumonia, but he refused to believe it was anything besides bronchitis. He left the ER and went home. When he left he said he wouldn’t tell his family because we had no proof. Unfortunately, he passed on a couple of weeks later.
90. Packed Up North
I’m a nurse. One night, I received a woman after her midwife let her go through eight hours of very difficult labor. In Canada, midwives practice separately from doctors and nurses. They have an agreement with hospitals to use the beds when labor becomes high risk. At this point, our doctors take over and plan an emergency c-section.
We realize the arteries in the sides of the uterus are ruptured due to extensive pushing. We delivered the baby fine, but the mom became a separate patient. Finally, the team finishes surgery but her blood pressure immediately plummets. They realize another artery is bleeding and that they needed to clamp her aorta.
This meant her lower body wasn’t receiving blood flow for several minutes. They replaced her blood volume a minimum of three times throughout. Finally, the team stabilized her but was afraid of anything else unexpected. The safest option was to pack her but leave the would open and send her to intensive care for further surveillance.
91. Defying The Lung Odds
Our patient came into the hospital with cystic fibrosis and end-stage lung function. He had an infection and was transferred to critical care after coughing blood, but began to code. There was panic everywhere. A major artery in his lung had eroded and he was bleeding out into his airway quickly. He had no chance of living without a transplant.
It was a long shot, and they performed the transplant after 10 days of him being kept alive. After a couple of weeks, he started to respond and was taken off assisted breathing equipment. He walked out of the hospital two months later and showed no complications a year later.
92. A Hole In The Plan
I’m a surgeon, and one patient had a brutal wound. When he got to the hospital we started CPR and blood transfusions, but we had to get a steady pulse to operate. We manage to get him on the table but lose the pulse again. I’m doing CPR while another surgeon locates an injury near his groin. At this point, I’m thinking we’re going to save this kid.
I didn’t realize as I continued CPR that the blood was just leaving through his groin wound. By now he’s been down about 20 minutes, and it’s just pouring out of the artery. That was the moment I knew this had gone downhill. We pause CPR to see if we have a pulse and there’s nothing. We had to call it. I’ll never forget how quiet the room was.
93. Quit Playing Games With My Heart
I worked as a mountain medic at a ski resort. Most of the time, I was treating people who fell on the mountain, and I had the rare occasions of an exciting broken femur. This was exciting because it meant their pants got cut off. On an even rarer occasion, you would have other medical events, but most people on skis are fit and healthy.
Most of the non-accident stuff happened at the lodge, and since the fire station was literally across the parking lot, they would just call them first. Their jump bags were better equipped for medical rather than trauma. One day, however, a call came about a heart attack and the firefighters weren't in the station due to hospital transportation.
A woman in her 40s had slipped and fallen on some ice. She appeared fine, but the lodge needed to medically clear her, so they called us down from our clinic at the upper lodge. We drove down on the snowmobile and start asking questions, palpating for broken bones or dislocated joints. She seems fine, but there is a slight weakness in her left arm.
I asked her history and any other symptoms and my partner flashed me her blood pressure. It was odd. Then she mentioned she was taking Tums. I asked why and she had woken up that morning with really bad heartburn. I then insisted she come with me to a private clinic room. She’s refusing, but I finally convince her that I'm not a doctor, and just being careful.
So we pop her shirt open and quickly get the monitor on, and confirm she's having a heart attack. I have no clue how she's standing, but women tend to have less of the big early symptoms and are tough as nails. We get her airlifted to the hospital and wait for news. The air medic told us after if she had waited any longer it could have been fatal.
94. And This Is Why We Wash Our Hands
Sometimes, surgeons are the ones in for an unpleasant surprise. My father is a physician and, although he's not a surgeon, he did some surgery while in medical school. He told me a story about a patient he had once who had necrotizing fasciitis—a.k.a. a really nasty flesh-eating disease. I almost wish that he hadn’t told me this story. It’s like something out of The Walking Dead.
The patient had gotten a cut while gardening and never cleaned the wound properly. My dad told us that he had to peel back layers just to get at it. First, he peeled off the bandages that the patient had self-applied. Then there was a layer of holy book pages that he also had to peel off. Layer upon layer, bandage upon bandage.
Finally, beneath all that, was the wound itself. No amount of med school training could have prepared my father for what he saw. The wound was covered in maggots. Apparently, they were eating the dead-tissue generated by the disease. He said that once they removed the maggots, they were able to begin the surgery to remove the infected areas.
Oddly enough, this patient had the maggots to thank for keeping his appendages intact. Because the maggots had eaten away the infected flesh, my dad and his team didn't have to amputate the patient’s limb. After this operation, though, my dad decided to not pursue surgery and focus on becoming a specialist.
95. The Big Heave
This happened to my brother while he was in med school. One day a guy strolled into the emergency room with the most extreme injury ever: He had the handle of a butcher blade sticking out from under one of his eyes. They did an X-ray on him and found that the whole blade was indeed in there, sticking into his skull.
Neurological tests also indicated that he was really lucky, as the blade didn't do any serious nerve or brain damage. After some debate, they decided to pull the blade out, but it was really stuck. Eventually, they laid the guy on his back, the ER doc took off his shoe, climbed up on the gurney, put his foot on the patient's forehead, and heaved the blade out.
They put the guy on the ward and the next morning, the authorities showed up to ask him about it. The guy just said, "Never mind, I'll take care of it". The next day, while no one was looking, the guy got up and walked out. For people who didn't show up for their yearbook photo, they substituted the X-ray of the guy with the blade in his head.
 Pexels
Pexels
96. Odd Anatomy
I’m a biomedical scientist, and my officemate was a medical doctor working on his PhD. He once did an appendectomy and cut into this person’s abdomen—only to find no appendix. He started freaking out. The support nurses in the room, however, started snickering at him because they knew right away what the problem really was.
Occasionally, they see someone with a rare genetic disorder where all their left-right asymmetries are reversed. This patient’s appendix was on the other side.
97. Didn’t Get The Memo
After my heart operation where they went in through my femoral artery, they forgot to tell anyone outside the theatre that they had given me anticoagulants. Long story short, when I got back to the ward, my mom and dad came to visit and see how I was doing—only to walk into a scene from a horror movie. I had two doctors and two nurses around me, caked in blood with the back wall of the room dripping with it.
I should have been in this tourniquet thing for like 12 hours minimum after surgery, but they removed it and asked me to get up and move around after four hours. Suffice to say, it wasn't pretty and the first nurse (the one who removed it) went absolutely white. No one answered the emergency buzzer for about 10-15 minutes to help her, either.
She just kept panicking and saying, "You are bleeding out!" to me. Oddly, I was completely calm and kept offering her advice. I think it was the shock, since I tend to get very analytical instead of scared. I should also mention that the advice I gave was rubbish: "Would you like me to hold that while you go and get some help?" She met this with, "You'll be a goner before I get back". "Oh ok, best for you to hold it then".
 Shutterstock
Shutterstock
98. A Telenovela Evening
One night while I was working in the Emergency room, a patient arrived with complaints of vaginal spotting. She told us she had been bleeding for two days and had a little pain. She thought it had started after her female partner had been “a little rough” during their last intimate experience. Her examination revealed something else entirely.
There was a complete tear and these injuries were consistent with a difficult childbirth. The story wasn’t adding up given the amount of trauma, so I ordered more tests, including a urine pregnancy test. The pregnancy test came back positive, which opened a huge can of worms, given her relationship status.
Turns out, she had secretly delivered a baby two days ago but didn’t tell anyone. She had been hiding the baby from her family and girlfriend. Everyone from child protective services to pediatrics got involved in the case. They found the baby in her apartment under some towels and it was a doozy of a night for paperwork. Her parents adopted the infant and as far as I know, they are still the child’s guardians.
99. A Tuesday In Radiology
I used to work for Radiology in a small hospital. We admitted a young couple in the middle of February who had been in a car accident. The girl gets a bed in the emergency room and she's overall fine. A few cuts and scrapes but still coherent and talking. A state trooper is in her room with her. Her partner is vocally complaining but stabilized on a spine board.
She asks if she can see him, but I tell her he can’t move and needs further tests. Well, she didn't like that one bit, and she begins to freak out as I take him to Radiology for a CT scan. The scan reveals an ugly result. The guy’s spine is severed. He’s in for serious surgery and rehab, and might never walk again. All of a sudden, though, the girlfriend runs into the room.
She’s tiny but squaring up to the cop, who ends up using his taser to get her under control. She gets cuffed to a bed for good measure. At the same time, they’ve just told her partner about his outcome and he is screaming her name. Later, we found out they were running product across the border and jeopardized more than just his spine that day.
100. A Tickle Under The Rib
I saw this one patient with a really odd condition. While she was asking me why she gets rib pain so often, she literally reached under her own rib and jiggled it with her fingers. Turns out, there were a lot of other things she could do that she shouldn’t ever be able to. I attributed it to a variant of Ehlers Danlos syndrome, which causes connective tissue abnormalities.
I was so distracted by the popping in and out of her rib that initially, I didn’t even notice how horrifying it was that she could get her hand under there.
101. Welcome To The World
My dad is a pediatrician specializing in neurological issues. He was seeing one of his patients at the hospital and got dragged into the NICU unexpectedly by a nurse who insisted that a baby wasn't well. The attending doctor insisted the kid was fine, and that he was just tired from a difficult vacuum assist delivery. My dad could tell the baby wasn't okay and managed to talk the parents into a brain scan.
The NICU doctor insisted my dad was nuts to the parents. Little did he know his arrogance would cost him, big time. The kid had a brain bleed and was rushed to surgery. The baby would not have lived without the nurse bringing my dad in and the parents listening to him. The delay caused by the NICU doctor almost certainly cost the kid some brain function. I’m proud that my dad did the right thing.
Sources: Reddit, , , , , , , , , ,